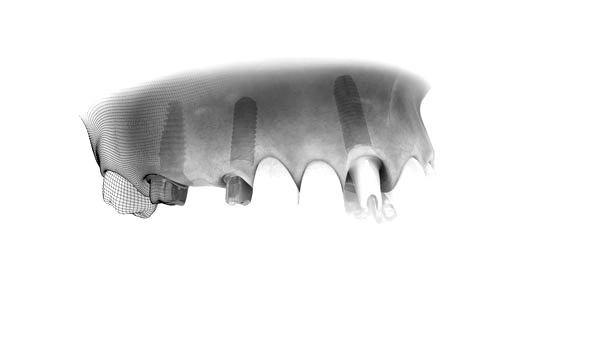
IMPLANTS DENTAIRES
Un implant dentaire sert à remplacer une dent manquante. Il s’agit d’une racine métallique, constituée d’un alliage de titane biocompatible, qui est insérée au sein de l’os de la mâchoire. Son rôle est de servir de fondation pour soutenir la nouvelle dent (couronne) qui sera par la suite confectionnée par un dentiste. Il est également possible de soutenir une prothèse dentaire complète et de stabiliser une prothèse dentaire partielle à l’aide de plusieurs implants.
Une fois l’implant placé dans la mâchoire, celui-ci se soude à l’os environnant. Il est si efficace que certains patients ont des implants en bouche depuis plus de quarante ans. En effet, le premier système commercial en implantologie a vu le jour en 1977.
La pose d’implant dentaire se fait sous anesthésie locale. Il est possible de bénéficier également d’une sédation intraveineuse lors de ce type d’intervention. Il est très rare qu’une anesthésie générale soit nécessaire. Dans ce cas, l’intervention doit se faire en milieu hospitalier.
Suite à sa pose, l’implant se soude progressivement à l’os. C’est pourquoi il faut respecter une période de guérison de deux à six mois suite à la mise en place d’un implant. La restauration finale de l’implant (pose de la couronne) ne peut se faire qu’après ce délai de guérison. Dans plusieurs cas, il est possible de quitter la clinique avec une restauration temporaire et ainsi éviter d’arborer un sourire sans dent. Si les conditions le permettent, cette restauration peut se faire directement sur l’implant. Sinon, une gouttière transparente peut supporter la restauration.
Suite à une extraction dentaire, l’os qui supportait la dent se résorbe progressivement au fil du temps. Lorsque l’os de soutien s’est trop aminci et qu’il est alors impossible d’y placer un implant, une greffe osseuse peut parfois être nécessaire afin de reformer l’os. Heureusement, de nouvelles technologies nous permettent souvent de ne pas avoir recours aux greffes osseuses.
Ajoutons que l’on peut remplacer plusieurs dents par un nombre inférieur d’implants. Pour stabiliser une prothèse à la mâchoire du bas, deux implants peuvent suffire. Pour ce qui est de supporter une prothèse complète à la mâchoire du haut, de 4 à 8 implants sont nécessaires.
EXTRACTIONS DENTAIRES
L’ablation de dents se déroule le plus souvent à la clinique sous anesthésie locale, avec ou sans sédation consciente. Dans certaines circonstances, une anesthésie générale peut être nécessaire, l’intervention se déroule alors en centre hospitalier.
EXTRACTION DES DENTS DE SAGESSE INCLUSES
Les troisième molaires, aussi appelées dents de sagesse, se retrouvent au nombre de quatre chez la majorité des gens. Elles sont situées au fond de chaque arcade dentaire, aux quatre coins de la bouche. Ce sont les dernières dents à faire éruption. Le positionnement adéquat de ces dents est souvent difficile étant donné un manque d’espace dans la bouche. Elles présentent typiquement une mauvaise orientation dans la mâchoire qui complique davantage leur éruption et empêchent qu’elles deviennent fonctionnelles et utiles.
Ces dents vont la plupart du temps faire éruption de façon partielle dans la bouche, on les qualifie alors de « semi-incluses ». Leur position éloignée et le repli de gencive qui les recouvre constituent une entrave à l’hygiène, ce qui favorise la mauvaise haleine, les infections locales et la perte d’os entre la dent de sagesse et la dent adjacente (défaut parodontal). Les dents de sagesse et les dents adjacentes sont aussi à risque de caries. Plus rarement, il est possible que la dent de sagesse cause la destruction de la dent adjacente (résorption).
Dans certains cas, les dents demeurent complètement incluses, c’est-à-dire qu’il n’existe aucune communication entre celles-ci et les bactéries de la cavité buccale. Bien que l’hygiène ne soit pas en jeu dans un cas comme celui-ci, il existe une faible possibilité de développer un kyste ou une tumeur au pourtour de la dent de sagesse. Il arrive également que les dents de sagesse se résorbent, ce qui provoque éventuellement une douleur sévère.
Pour toutes ces raisons, lorsque c’est indiqué, il est préférable de procéder à l’extraction des dents de sagesse de façon préventive ou curative, entre les âges de 15 et 25 ans. En effet, il est démontré que l’intervention est plus complexe et présente davantage de complications à mesure que le patient vieillit.
Les complications les plus fréquentes sont l’infection post-opératoire et l’alvéolite. Plus rarement, l’extraction d’une dent de sagesse du haut peut provoquer une communication avec le sinus, et l’extraction d’une dent de sagesse du bas peut engourdir une partie de la lèvre inférieure de façon temporaire ou permanente.
Les chirurgiens de la Clinique Maxillo-Mauricie vous aideront à prendre la meilleure décision concernant vos dents de sagesse: extraire ou observer? Lorsque les dents ne causent pas de symptômes, il s’agit-là d’un dilemme auquel nous sommes confrontés régulièrement.
Lors de la consultation initiale, le chirurgien révisera l’histoire médicale et dentaire. Une attention particulière sera portée à tout symptôme que le patient croit associé aux dents de sagesse. Un examen clinique détaillé est ensuite effectué. L’examen radiologique de base est le panorex, mais il se peut qu’une radiographie en trois dimensions soit recommandée (« scan »). Ces images nous permettent entre autres d’évaluer la position des dents de sagesse et leur relation aux dents adjacentes, au sinus et au nerf alvéolaire inférieur.
Les éléments recueillis lors de la consultation permettent au chirurgien de convenir avec le patient d’une conduite à tenir, en tenant compte des risques et des bénéfices que chaque décision comporte. Vous recevrez des explications détaillées concernant tout ce qui vous préoccupe.
L’extraction des dents de sagesse est une intervention simple, mais dont la perspective provoque de l’anxiété chez la plupart des patients. C’est l’une des raisons pour lesquelles nous offrons la sédation intra-veineuse, qui permet l’administration de médicaments qui détendent efficacement, en plus de réduire l’enflure et la douleur post-opératoire. À noter par ailleurs qu’une anesthésie locale permet une procédure sans douleur.
EXPOSITION DE DENTS INCLUSES
Il arrive que certaines dents (le plus souvent des canines) demeurent coincées sous la gencive et qu’il leur soit impossible de faire éruption au bon endroit. Il peut être souhaitable de ne pas les enlever. On peut permettre une éruption de ces dents grâce à une chirurgie, combinée à un traitement orthodontique. Lorsque l’intervention se déroule au bloc opératoire (en centre hospitalier, sous sédation consciente ou sous anesthésie générale), les coûts en sont payés par la RAMQ. Il s’agit d’une procédure tout à fait envisageable à la clinique sous anesthésie locale, mais le patient doit alors payer les honoraires.
APECTOMIE
Intervention qui consiste à retirer l’infection au bout de la racine d’une dent dont le traitement de canal a échoué. L’intervention se déroule le plus souvent à la clinique sous anesthésie locale, avec ou sans sédation consciente.
BIOPSIE
Intervention visant à enlever en partie ou en entier une lésion (tissu dont l’apparence diffère de la normale) afin d’en permettre l’analyse et l’identification par un pathologiste. L’intervention se déroule le plus souvent à la clinique sous anesthésie locale, avec ou sans sédation consciente. Dans certaines circonstances, une anesthésie générale peut être nécessaire, l’intervention se déroule alors en centre hospitalier.
SÉDATION INTRAVEINEUSE ET INTRA-MUSCULAIRE
Méthode de gestion de l’anxiété par l’administration de médicaments sédatifs (qui aident à se détendre sans endormir complètement).
